Coming home after laparoscopic surgery and feeling sore, bloated, uncomfortable in the abdomen or abdominal pain after laparoscopic surgery is not a sign that something went wrong. It is one of the most common things patients experience in the first few days of recovery — and in the vast majority of cases, it settles on its own with the right approach.
The reason patients are often caught off guard is that laparoscopic surgery carries a reputation for being “minimally invasive” and easy to recover from. That part is true when you compare it to open surgery. But the abdomen has still been through a procedure. Gas was introduced, instruments were passed in, organs were moved around. The body responds to all of that — and abdominal discomfort is part of that response.
Dr. Harsh Sheth, MS (General Surgery), FMAS, FIAGES — a laparoscopic and bariatric surgeon in Mumbai at Genèse Clinic with over 10 years of surgical experience and more than 5,000 minimally invasive procedures performed — walks patients through this exact concern regularly. This guide brings together everything he advises patients on, in one place.
Why Does Abdominal Pain Occur After Laparoscopic Surgery?
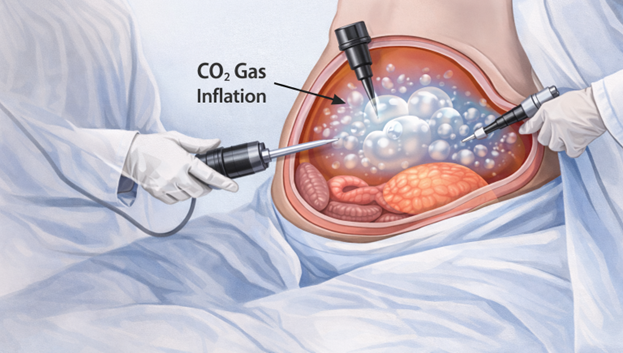
Understanding the source of the pain is the first step toward managing it effectively. Post-operative abdominal discomfort after laparoscopic surgery generally comes from three distinct causes.
Residual Carbon Dioxide Gas
During every laparoscopic procedure, the abdomen is inflated with carbon dioxide gas. This creates the working space that allows the surgeon to see clearly and manoeuvre instruments safely. At the end of the surgery, as much gas as possible is removed — but small amounts inevitably remain trapped in the abdominal cavity.
This residual CO₂ is the most common cause of post-operative discomfort. It irritates the diaphragm and the inner abdominal lining, causing cramping, bloating, and a heavy, pressured feeling in the abdomen. It also causes referred pain in the shoulders and upper back — something that surprises many patients because it seems completely unrelated to their surgery site.
Incision Site Soreness and Swelling
Laparoscopic port cuts are small — typically between 0.5 and 1.5 centimetres — but the tissue surrounding each incision still experiences trauma. Localised swelling, bruising, and tenderness at each port site are entirely expected and form part of normal tissue healing. Patients often interpret this soreness as a sign of complications, when in reality it is simply the wound repair process underway.
Temporary Slowdown in Gut Activity
The abdominal organs do not respond well to being displaced and handled, even by skilled hands during a minimally invasive procedure. Combined with the effects of general anaesthesia, bowel motility commonly slows down in the first 24 to 72 hours after surgery. This leads to gas accumulation, cramping, a feeling of fullness or pressure, and occasionally nausea — all of which contribute to the overall abdominal discomfort patients feel during early recovery.
How to Manage Abdominal Pain After Laparoscopic Surgery

The following strategies are what Dr. Harsh Sheth recommends to patients recovering from laparoscopic procedures including gallbladder removal, hernia repair, appendix surgery, and bariatric surgery in Mumbai. These are practical, evidence-backed steps that make a real difference to comfort and recovery speed.
Start Walking Early — Even Short Distances
Why It Helps
Walking is the single most effective thing you can do for post-operative abdominal pain. Gentle movement stimulates peristalsis — the natural wave-like contractions that move gas and waste through the gut. It directly addresses one of the three primary causes of pain by helping the digestive system return to its normal rhythm faster.
Walking also reduces the risk of blood clots, maintains circulation to healing tissue, and prevents the muscle stiffness that can worsen overall discomfort.
How to Do It
Start with just five to ten minutes of slow walking around the room or corridor within 12 to 24 hours of returning home, provided your surgeon has cleared you for gentle mobilisation. Aim for three to four short walks spread across the day rather than one long session. Build duration gradually as comfort improves. The goal is consistency, not intensity.
Apply a Warm Compress to the Abdomen
Why It Helps
Heat is a well-established aid for abdominal cramping and muscle tension. Applied to the abdomen after laparoscopic surgery, warmth relaxes the abdominal wall muscles that often tighten involuntarily around the surgical area, eases gas cramping, and improves local blood flow to support tissue repair.
Many patients also find a warm compress on the shoulder and upper back helpful for the referred pain caused by diaphragm irritation from CO₂ gas.
How to Do It
Use a covered heating pad or a cloth-wrapped warm water bottle. Apply for 15 to 20 minutes at a time, up to three or four times per day. Always maintain a fabric layer between the heat source and skin to avoid burns. Avoid placing direct heat over any fresh incision site.
Follow a Careful Post-Surgery Diet
Why It Matters
The digestive system after a laparoscopic procedure operates below its normal capacity for several days. Eating the wrong foods during this window increases gas production, adds pressure to the abdominal cavity, and significantly worsens discomfort.
What to Eat
For the first 24 to 48 hours, focus on clear fluids — plain water, diluted fruit juices, thin soups, and herbal teas. As tolerance improves over days two to four, transition to soft, easily digestible foods such as khichdi, curd rice, soft cooked vegetables, plain dal, and bananas. Eat small portions frequently rather than full meals.
What to Avoid
During the first week of recovery, avoid carbonated drinks of any kind, beans and heavy lentil preparations, raw cruciferous vegetables such as cabbage, cauliflower, and broccoli, greasy or heavily spiced food, and large meal portions. These foods either generate excess gas or require more digestive effort than your gut is ready for in the immediate post-operative period.
Stay Consistently Hydrated
Why It Matters
Adequate hydration after minimally invasive surgery supports the flushing of residual anaesthetic agents from the body, maintains bowel motility, reduces constipation risk, and supports tissue healing at the cellular level.
How Much to Drink
Eight to ten glasses of plain water per day is a reasonable baseline for most adult patients, unless Dr. Harsh Sheth has given you specific fluid restrictions based on your procedure. Warm water is generally gentler on the digestive system than cold water in the first few post-operative days. Sip consistently throughout the day rather than drinking large amounts at once.
Avoid caffeinated beverages and all fizzy drinks until the bloating has fully resolved.
Take Prescribed Medications as Directed
Understanding Your Prescription
Dr. Harsh Sheth prescribes a personalised post-operative pain management plan based on the specific procedure performed and each patient’s medical history. This typically includes a combination of anti-inflammatory agents, mild analgesics, and antispasmodics.
The most important principle of post-operative pain medication is staying ahead of the pain. Taking medication on schedule — rather than waiting for pain to become severe — maintains a stable therapeutic level in the body and keeps discomfort in a manageable range throughout the day.
Additional Options
Simethicone, available over the counter at most pharmacies, helps break down gas bubbles in the digestive tract and can ease gas-related cramping and bloating. Always confirm with Dr. Harsh Sheth before adding any over-the-counter medication to your post-operative regimen.
Unless specifically cleared by your surgeon, avoid non-steroidal anti-inflammatory drugs such as ibuprofen, as they can irritate the stomach lining, which is already under stress from surgery and anaesthesia.
Adjust Your Resting Position
Why Position Matters
Lying completely flat after laparoscopic surgery can increase pressure on the diaphragm and worsen gas-related discomfort. Small adjustments to resting posture can make a meaningful difference to comfort levels.
Recommended Positions
Lying on the left side with a pillow placed between the knees encourages gas to move naturally through the digestive tract. A semi-reclined position, supported by two to three pillows under the upper back and head, reduces abdominal pressure while allowing the gut to function more comfortably.
When sitting upright, maintain a straight spine rather than hunching forward. When you need to cough, laugh, or sneeze, press a small folded pillow firmly against your abdomen to reduce strain on incision sites and the abdominal wall — this small technique, known as splinting, is standard advice after any abdominal procedure.
Practice Deep, Deliberate Breathing
Why It Helps
After abdominal surgery, it is common for patients to unconsciously restrict their breathing to avoid moving the abdominal muscles. This shallow breathing pattern slows the absorption and expulsion of residual CO₂ and increases tension in the abdominal wall — both of which worsen discomfort.
How to Do It
Diaphragmatic breathing — breathing in slowly through the nose while allowing the belly to gently expand, then exhaling slowly through the mouth — encourages deeper respiratory exchange and helps the body process trapped gas more efficiently. It also activates the parasympathetic nervous system, which reduces pain perception.
Practise five to ten slow, deep breaths in this way, three to four times daily. It is particularly helpful first thing in the morning and before sleep.
Prevent and Address Constipation Early
Why Constipation Is a Hidden Cause of Abdominal Pain
Constipation is among the most underreported contributors to post-operative abdominal discomfort. It is also one of the most common, affecting a significant proportion of patients after laparoscopic surgery due to the combined effects of general anaesthesia, reduced mobility, dietary changes, and pain medication — particularly opioid-based analgesics, which slow bowel function as a side effect.
What to Do
Walk regularly. Drink warm water consistently — a glass of warm water with a squeeze of lemon first thing in the morning can gently stimulate bowel activity. Soft stewed prunes and ripe bananas are natural, gentle aids. If you have not passed stool within two to three days of surgery despite these measures, contact Dr. Harsh Sheth’s team at Genèse Clinic for guidance on whether a mild laxative is appropriate.
Straining forcefully against constipation puts significant mechanical pressure on abdominal incisions. Avoid this at all costs during the early recovery period.
Prevent and Address Constipation Early
Why Constipation Is a Hidden Cause of Abdominal Pain
Constipation is among the most underreported contributors to post-operative abdominal discomfort. It is also one of the most common, affecting a significant proportion of patients after laparoscopic surgery due to the combined effects of general anaesthesia, reduced mobility, dietary changes, and pain medication — particularly opioid-based analgesics, which slow bowel function as a side effect.
What to Do
Walk regularly. Drink warm water consistently — a glass of warm water with a squeeze of lemon first thing in the morning can gently stimulate bowel activity. Soft stewed prunes and ripe bananas are natural, gentle aids. If you have not passed stool within two to three days of surgery despite these measures, contact Dr. Harsh Sheth’s team at Genèse Clinic for guidance on whether a mild laxative is appropriate.
Straining forcefully against constipation puts significant mechanical pressure on abdominal incisions. Avoid this at all costs during the early recovery period.
When Abdominal Pain After Laparoscopic Surgery Needs Medical Attention
Routine post-operative discomfort should improve steadily and noticeably from day two or three onward. If your pain trajectory is moving in the opposite direction — or if you notice any of the following symptoms — contact Dr. Harsh Sheth at Genèse Clinic or seek medical attention promptly rather than waiting:
Worsening pain that is getting sharper or more intense rather than gradually improving
Fever above 38°C combined with abdominal pain or tenderness
Signs of infection at any incision site — redness, warmth, unusual swelling, or discharge
Inability to pass gas or stool for more than two to three days post-surgery

Rigidity of the abdomen — a hard, board-like feel that was not present in the first day
Persistent nausea or vomiting that is not settling with time
Shortness of breath or chest discomfort of any kind
These symptoms can indicate complications including surgical site infection, internal bleeding, or bowel obstruction. Complications after laparoscopic surgery are uncommon, but they require prompt evaluation when they do occur. Do not attempt to manage these at home.
Recovery After Laparoscopic Surgery — What to Expect Day by Day

Day | What Is Typical |
Day 1–2 | Gas cramping, shoulder pain, incision soreness, fatigue, low appetite |
Day 2–3 | Gas pain begins easing, light food tolerated, short walks manageable |
Day 3–5 | Bloating reduces significantly, bowel activity returns, energy improves |
Day 5–7 | Most patients comfortable on light oral pain relief only |
Week 2 | Return to light daily activities for most patients |
Week 4–6 | Full recovery for most laparoscopic procedures |
Individual timelines vary depending on the type of procedure, patient age, overall health, and adherence to post-operative guidance.
Expert Laparoscopic and Bariatric Surgery at Genèse Clinic, Mumbai
Dr. Harsh Sheth, MS (General Surgery), FMAS, FIAGES, has dedicated over a decade to advancing minimally invasive surgery outcomes for patients across Mumbai. His areas of surgical focus include laparoscopic gallbladder removal, hernia repair, appendix surgery, bariatric and weight loss surgery, and complex abdominal procedures — all performed with an emphasis on precision, safety, and supported recovery.
At Genèse Clinic in Mumbai, every surgical patient receives a clear, personalised post-operative care plan before they leave the facility. Recovery support does not end at the operating table.
If you are currently recovering from a laparoscopic procedure and have concerns about your abdominal pain — or if you are preparing for an upcoming surgery and want to understand the recovery process in full — the team at Genèse Clinic is available to help.
Frequently Asked Questions
1. How long does abdominal pain last after laparoscopic surgery?
Gas-related cramping — the most intense component of post-operative abdominal discomfort — typically resolves within one to three days as the body absorbs and expels residual CO₂. General abdominal soreness and incision tenderness may persist for five to seven days. If pain is not improving by day five or is actively worsening at any point, contact your surgeon for evaluation.
2. Is bloating and heaviness in the abdomen normal after laparoscopic surgery?
Yes, completely. The CO₂ gas introduced during the procedure and the temporary reduction in bowel motility after anaesthesia both contribute to that bloated, heavy feeling. Consistent walking, light eating, and staying hydrated are the three most effective things you can do to help this resolve as quickly as possible.
3. Can I use a heating pad on my abdomen after laparoscopic surgery?
Yes. A warm compress or covered heating pad applied to the abdomen provides genuine relief from gas cramping and muscle tension. Use it for 15 to 20 minutes at a time, maintain a cloth layer between the heat source and your skin, and avoid applying heat directly over fresh incision sites.
4. Which foods make abdominal pain worse after laparoscopic surgery?
Carbonated drinks, beans, raw cruciferous vegetables, fried food, and heavy spiced preparations are the main offenders — all increase gas production and put additional strain on the digestive system during a period when it needs to recover. Stick to soft, easy-to-digest foods for the first week and reintroduce your normal diet gradually over the following days.
5. When should I contact Dr. Harsh Sheth about abdominal pain after surgery?
Contact Genèse Clinic if you develop fever, sharply worsening or severe pain, signs of infection at the incision sites, inability to pass gas or stool beyond two to three days, or any breathing difficulty or chest discomfort. These symptoms require prompt medical review rather than home management.